ICU, NICU, PICU & Critical Care Design in India
An Architect's Working Reference — Open-Bay vs Single-Cubicle ICU, NICU and PICU Specifics, Isolation Cluster, BMT Positive-Pressure, Acuity-Adaptable Rooms, Family Presence, Monitoring Lines, Pressure Cascades, and the Critical-Care Architectural Toolkit
Critical care units are the most monitored, most equipped, and most family-occupied spaces in a hospital. They are also the architectural typology where international and Indian practice diverge most consistently — international tertiary practice has moved decisively toward single-room ICU and single-room NICU; Indian practice continues to operate predominantly open-bay configurations for cost, observation efficiency, and the joint-family caregiving culture. The architect on a critical-care commission must make this choice consciously rather than by default, with awareness of the outcomes evidence on either side.
This guide is the third in the design-focused series. It covers adult ICU, NICU (neonatal), PICU (paediatric), specialty critical-care variants (cardiac ICU, neuro ICU, BMT, isolation cluster), and the family-centred care framework that has emerged as the dominant international design paradigm and is now informing the better Indian projects. The guide assumes the reader has read the pillar regulatory reference, the regulatory deep-dives, and the preceding design-series articles on clinical adjacencies and OT suite design.
"The intensive care unit is where the building's mechanical systems and the patient's biology meet. It is not a room. It is a machine — a machine into which a small number of human beings are temporarily inserted." — Dr. Devi Shetty (b. 1953), cardiac surgeon and founder Narayana Health, paraphrased from a 2014 design review
"Critical care medicine has improved survival to such a degree that the next frontier is no longer mortality but morbidity, and architecture has a direct role in morbidity — through noise, light, sleep, infection, and family stress." — Dr. Hannah Wunsch, intensivist and researcher, paraphrased from Critical Care Medicine (2014)
1. The ICU Architectural Spectrum
Critical care is not a single typology. It spans an architectural spectrum from low-acuity HDU to ultra-isolation BMT, with distinct design requirements at each level.
| Unit | Acuity | Patient Population | Architectural Pattern |
|---|---|---|---|
| HDU (High Dependency Unit) | Step-down from ICU | Stable but monitored | 8–10 m²/bed; open bay or 4-bed cubicle |
| General Adult ICU (MICU/SICU) | High | Medical / surgical critically ill | 9–14 m²/bed; open bay (Indian) or single (intl.) |
| Cardiac ICU (CCU/CTICU) | High | Post-cardiac surgery; cardiac event | 12–14 m²/bed; cardiac-specific monitoring |
| Neuro ICU | High | Neuro-surgery, stroke | 12–14 m²/bed; quiet; reduced light |
| Burns ICU | High | Burn injury | 14–18 m²/bed; HEPA; humidity 60% |
| Trauma ICU | High | Trauma; multi-organ | 14 m²/bed; ED-adjacent |
| NICU | Highest (neonatal) | Newborns < 28 days, premature | 10–14 m²/bay; 4–6 bay open or single room |
| PICU | Highest (paediatric) | Children critically ill | 12–16 m²/bay; family presence |
| BMT (Bone Marrow Transplant) | Highest (immunocompromised) | Transplant patients | 16–20 m²/room; HEPA + positive pressure |
| Isolation (negative-pressure) | High (infectious) | TB, COVID-type, multi-drug-resistant | 16 m²/room; anteroom + HEPA exhaust |
A 100-bed hospital typically has: 8–12 ICU beds (general), 4–6 HDU, 1–2 isolation, 4–6 NICU (if obstetric); a 200-bed adds: 6–8 cardiac, 2–4 neuro, 4–6 PICU. A 500-bed tertiary adds: BMT 6–8, burns 6–10, expanded ICU clusters.
2. Open-Bay vs Single-Cubicle vs Single-Room — The Architectural Spectrum
Three distinct adult-ICU architectural patterns exist; the choice is consequential.
| Pattern | Bay Size | Beds per "room" | Visibility | Privacy | Cost | Indian Use |
|---|---|---|---|---|---|---|
| Open bay | 9–12 m²/bed | 6–12 beds in one space | High (single nurses' station sees all) | Low (curtains only) | Low | Most common; default |
| Cubicle / pod | 10–12 m²/bed | 4–6 beds with low-wall partition | Moderate | Moderate | Moderate | Increasingly common |
| Single room (with glazed front) | 14–18 m²/room | 1 | Direct via glass front | High | Higher | Tertiary private; growing |
| Single room (closed) | 16–20 m²/room | 1 | Via monitor / wall window | Very high | Highest | International norm; rare in India |
The evidence:
- Single-room ICU outcomes (international studies: Stiller, 2008; Gabor, 2003) — lower cross-infection, reduced delirium, better sleep, higher family satisfaction; higher staff walking distance, longer time-to-bedside.
- Open-bay ICU — faster nursing response, easier sharing of equipment and senior oversight, lower capex; higher cross-infection risk, lower sleep quality, lower privacy, higher noise.
The Indian calculus: open-bay is operationally efficient and matches the joint-family caregiving culture (where families want to see other patients and other nurses, not isolation); single-room is clinically superior for outcomes and aligns with international tertiary practice. The architect's recommendation depends on the project's positioning — tier-2 community hospital favours open-bay; tertiary specialty hospital favours single-room or cubicle; teaching hospital often hybrid (open-bay for teaching, single-room for isolation).
3. Adult ICU — Architectural Specifications
| Element | Specification |
|---|---|
| Bed area (open bay) | 9 m² minimum (NABH); 12 m² preferred |
| Bed area (single room) | 14–18 m² with toilet, family chair, sink |
| Inter-bed clearance | 1.8 m minimum (NABH); 2.4 m preferred |
| Foot clearance | 1.2 m minimum for cart access |
| Headwall | Per bed: O2 ×2, Air ×1, Vacuum ×3, gas outlets to NIST/DIN; 14–18 power outlets (UPS-backed); 2× nurse-call; data port; lighting controls; suction |
| Lighting | Ambient 200–400 lux; examination 1000 lux; reading 500 lux; circadian (warmer evening); patient-controlled |
| Floor finish | Welded vinyl; antimicrobial; coved skirting; impact-resistant |
| Wall finish | PVC panel or epoxy-painted; antimicrobial; impact-resistant at trolley height |
| Ceiling | Sealed; gypsum with epoxy or modular metal; sprinkler-compatible |
| Ceiling height | 3.0 m minimum; 3.3 m preferred for ceiling-mounted equipment |
| Doors | Glazed sliding doors for single rooms; manual swing for open bay |
| Glazing | Full-height to nurses' station / corridor for visibility |
| Privacy | Curtain (open bay); blind/curtain (single); glazed shutter |
| Hand-wash | Sensor-tap basin per 2 beds (open bay); 1 per single room |
| Hand-rub dispenser | At each bed entry |
| Toilet | En-suite for single rooms; cluster toilets for open bay |
| Family chair | One recliner per bed; pull-out for sleep optional |
| Patient lift / hoist | Ceiling-mounted track per bed (preferred) or mobile |
| Isolation provision | At least 1 negative-pressure isolation per ward unit (NABH) |
| BMT cluster | 4–6 beds in HEPA + positive-pressure cluster |
Headwall design:
The headwall is the architectural-mechanical interface where most ICU services converge. Modern best practice uses a modular pre-fabricated headwall (metal panel with integrated gas outlets, power, lighting, monitor mount) that is delivered as a single unit and installed against a structural wall. Field-built headwalls (gas outlets installed individually in plastered wall) are cheaper but less reliable.
4. The ICU Nurses' Station — Visual Control Geometry
The nurses' station is the architectural pivot of the ICU. Its placement determines visibility, response time, and family / staff interaction.
| Pattern | Placement | Visibility | Application |
|---|---|---|---|
| Central | Centre of open bay | All beds visible | Open-bay 6–10 beds |
| Pod-and-station | One station per 4–6 bed pod | Each pod independently observed | Cubicle / pod |
| Linear corridor | Stations along corridor | Single rooms via glazed front | Single-room ICU |
| Decentralised micro-stations | One mini-station per 2–4 rooms | Highest staff proximity | Newer single-room designs |
Sizing:
- Central station: 12–18 m² for 6–10 beds; nurse computer × 2, patient monitor wall, charting space, telephone, supplies
- Per-pod micro-station: 4–6 m² with workstation + medication trolley parking
- Visual control rule: every patient bed must be visible from at least one nurses' station with a sight line ≤ 12 m and ≤ 5 second walk
5. NICU — The Most Specialised Critical Care
Neonatal intensive care is the architectural typology that has changed most over the last 20 years. International practice has moved from the open ward (Florence-Nightingale-derived) to single-family rooms (developmental care).
| NICU Pattern | Layout | Patient Density | Family Provision |
|---|---|---|---|
| Open bay (4-bay or 6-bay) | Cots in one room with curtains | Higher | Low — visiting hours |
| Single-family room (SFR) | One room per baby, family 24×7 | Lower | High — overnight |
| Hybrid | Mix of open and SFR | Moderate | Moderate |
The developmental-care evidence (Lasky 2009, White 2013):
- Single-family room reduces noise, light, parental stress
- Improved infant weight gain, earlier discharge
- Higher staff walking distance, requires more nurses
- Family presence increases breastfeeding, reduces re-admission
Indian context: SFR NICU is rare due to footprint and operational cost; most Indian NICUs are open-bay 4-6 cot. The architect designing a new NICU should evaluate hybrid (4-cot open bay + 4 single rooms for special cases).
NICU specifications
| Element | Specification |
|---|---|
| Cot area (open bay) | 6–8 m² per cot |
| Cot area (single room) | 14–18 m² per room with parent chair |
| Inter-cot spacing | 1.8 m minimum; 2.4 m preferred |
| Overhead lighting | Dimmable to ≤ 5 lux for sleep; 200 lux for procedures; circadian |
| Examination lighting | 2000 lux at cot for procedure |
| Sound | Average ≤ 45 dB; peak ≤ 65 dB; sound-absorbing ceiling and walls |
| Temperature | 24–26°C |
| Humidity | 45–60% |
| Air changes | ≥ 6 ACH outside; positive pressure |
| HEPA | H13 filtration |
| Hand-hygiene | Sensor basin at every 2 cots; alcohol-rub at every cot |
| Family seating | Recliner chair adjacent to every cot; kangaroo-care space |
| Breast-feeding / pumping room | 9–12 m²; private; comfortable |
| Milk preparation | 6 m²; pasteurisation, refrigerator, sealed |
| Phototherapy area | If used; eye-protection signage |
| Resuscitation cot | Adjacent to delivery suite |
| Step-down nursery | For graduating babies; 4–6 cots |
| Isolation NICU room | 1 minimum; HEPA exhaust |
The kangaroo-care space: unique to NICU — a parent-and-baby skin-to-skin contact zone with reclining chair, blanket warmer, and privacy. Indian context has high cultural fit (extended family supports prolonged kangaroo presence). Architect designs 2–4 m² per cot for this.
6. PICU — Paediatric Specifics
| Element | PICU Specification |
|---|---|
| Bed area | 12–16 m²; family chair + study area |
| Inter-bed | 1.8 m minimum |
| Layout | Mix of open bay and single rooms; older children prefer single |
| Wall finish | Cheerful colours; child-friendly graphics (institutional grade) |
| Lighting | Lower intensity at night; child-controllable for older patients |
| Headwall | Same as adult ICU |
| Toy / activity space | If extended stay |
| Family room | Adjacent; sleeping arrangement |
| Bath / shower | Family-accessible |
| Dietary | Child-friendly menu space |
PICU sits between NICU's developmental specifics and adult ICU's clinical generality. Architect treats it as an adult ICU with paediatric overlays.
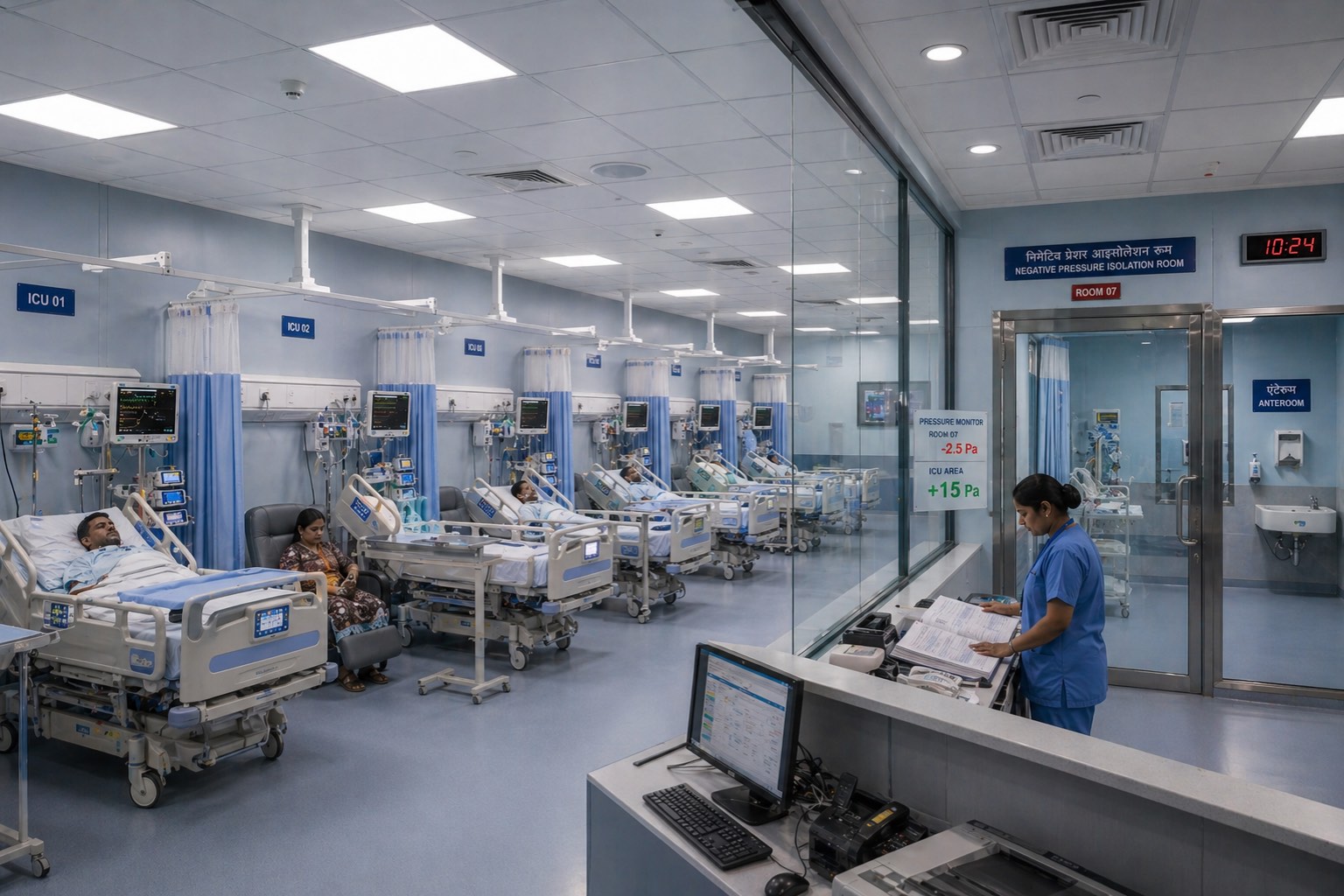
7. Isolation Cluster and BMT Architecture
| Type | Pressure | HVAC | Application |
|---|---|---|---|
| Negative-pressure isolation | − 5 to − 15 Pa | HEPA exhaust to roof; 12+ ACH | TB, COVID-type, MDR |
| Positive-pressure isolation | + 8 to + 15 Pa | HEPA supply; positive | BMT, immunocompromised, post-transplant |
| Combined / convertible | Switchable | Bi-directional dampers | Dual-purpose |
Negative-pressure isolation room
| Element | Specification |
|---|---|
| Room area | 14–18 m² + anteroom 4.5–6 m² |
| Anteroom | Always required; PPE donning/doffing; hand-wash basin |
| Air changes | ≥ 12 ACH; HEPA H14 exhaust to roof |
| Pressure differential | ≥ 2.5 Pa negative to anteroom |
| Door | Self-closing; sealed gasket |
| Window | Sealed; double-glazed |
| En-suite toilet | Pressure-negative; sealed |
| Pressure monitor | Continuous, visible at door |
| Communication | Intercom + phone |
Positive-pressure BMT room
| Element | Specification |
|---|---|
| Room area | 16–20 m² + anteroom 5 m² |
| Anteroom | Always required; gowning |
| Air changes | ≥ 12 ACH supply; HEPA H14 |
| Pressure differential | ≥ 2.5 Pa positive to anteroom |
| Filtration | HEPA + ULPA at terminal |
| Surfaces | Smooth, jointless; epoxy or PVC panel |
| Furniture | Sealed, washable |
| Family chair | Optional; restricted visiting |
| Reverse-isolation toilet | Pressure-positive; sealed |
| Diet | HEPA-handled |
The BMT cluster of 4–6 rooms is typically a separate unit within ICU or as a dedicated wing. Its HVAC and structural requirements are higher than general ICU.
8. Pressure Cascade and HVAC for Critical Care
| Critical-Care Space | Pressure (Pa) | ACH | Filtration |
|---|---|---|---|
| Adult ICU general | + 5 | ≥ 6 | HEPA H13 preferred |
| Cardiac ICU | + 5 | ≥ 6 | HEPA H13 |
| Neuro ICU | + 5 | ≥ 6 | HEPA H13 |
| NICU | + 5 to + 8 | ≥ 6 | HEPA H13 |
| PICU | + 5 | ≥ 6 | HEPA H13 |
| BMT positive | + 8 to + 15 | ≥ 12 | HEPA H14 + ULPA |
| Isolation negative | − 5 to − 15 | ≥ 12 | HEPA H14 exhaust |
| Anteroom (BMT) | Intermediate positive | ≥ 6 | HEPA |
| Anteroom (isolation) | Intermediate negative | ≥ 6 | HEPA |
| ICU corridor | Neutral / 0 | ≥ 6 | HEPA H13 |
| Soiled utility | − 5 | ≥ 6 | Standard |
The pressure cascade is the architectural-engineering core of critical-care HVAC. Architect coordinates with HVAC consultant at preliminary design.
9. Acuity-Adaptable Rooms — The Future Direction
International best practice is increasingly moving toward acuity-adaptable patient rooms — single rooms that can scale from general ward (low acuity) to ICU (high acuity) without patient transfer. The patient stays; the equipment changes.
| Acuity-Adaptable Element | Specification |
|---|---|
| Room area | 18–24 m² (ICU-sized) |
| Headwall services | Full ICU spec (can scale up) |
| Floor / wall finish | ICU spec |
| Lighting | Full ICU spec |
| Patient lift | Ceiling-mounted track |
| Family chair / sleep | Full ICU spec |
| HVAC | ICU spec; adjustable pressure |
| Equipment delivery | Modular; rolled in for upgrade |
| Cost | 30–50% above general ward; 10–20% below dedicated ICU |
Argument for: reduces inter-unit transfers (associated with morbidity), reduces family disruption, future-proofs the building for evolving care patterns.
Argument against: higher upfront capex, equipment under-utilisation if patient stable, requires nursing skill range.
Indian context: acuity-adaptable is rare; tertiary private hospitals are starting to provision a small "convertible" cluster of 4–6 rooms. Architect should propose this for new tertiary projects.
10. Family Presence and Family-Centred Care
Indian critical-care is uniquely family-intensive. The architect's design must accommodate this rather than design against it.
| Family Provision | Specification |
|---|---|
| Family chair / recliner per bed | Yes — comfort, sleeping if needed |
| Family overnight space | Within ICU (single room) or adjacent (open bay) |
| Family lounge per ICU | 25–60 m² with seating, water, TV, charging, restroom |
| Family education room | 12–18 m² for counselling, end-of-life discussions |
| Spiritual / prayer space | Adjacent to ICU (at least multi-faith room) |
| Visitor toilets / shower | Per ICU |
| Pantry / refreshment | Per ICU |
| Family-staff communication | Daily updates, scheduled rounds, white-board, language access |
The family-centred care framework, articulated by the Society of Critical Care Medicine and adopted in NABH 5th edition, treats the family as a member of the care team rather than a visitor. Indian practice has always treated the family this way; international practice is converging.
11. Common Critical-Care Failure Modes
| # | Failure | Prevention |
|---|---|---|
| 1 | Bed area < 9 m² | NABH minimum 9 m²; design 12 m² |
| 2 | No isolation in ICU | At least 1 negative-pressure per ICU |
| 3 | No anteroom for isolation / BMT | Anteroom always required |
| 4 | Single-corridor ICU without service-side access | Service corridor for trolleys |
| 5 | Nurses' station without sightlines to all beds | Visual-control rule |
| 6 | Headwall field-built rather than modular | Pre-fabricated headwall |
| 7 | Family seating absent | Recliner per bed minimum |
| 8 | Hand-hygiene basin frequency < 1 per 2 beds | NABH spec |
| 9 | Lighting not dimmable / circadian | Patient-controlled, dimmable |
| 10 | Floor not welded vinyl | Welded; coved skirting |
| 11 | NICU lighting not dimmable to ≤ 5 lux | Dimmable for sleep |
| 12 | NICU sound > 45 dB | Sound-absorbing surfaces |
| 13 | BMT without HEPA + positive pressure | Full BMT spec |
| 14 | Acuity-adaptable absent in tertiary | Provision a 4-6 room cluster |
| 15 | Family lounge undersized or absent | 25–60 m² per ICU |
| 16 | Multi-faith / prayer / counselling room absent | Required ≥ 100 beds |
| 17 | Pressure monitor absent at isolation door | Continuous monitor |
| 18 | Patient lift absent — manual lifting | Ceiling-mounted track |
12. The Architect's Critical-Care Design Toolkit
| # | Step | Output |
|---|---|---|
| 1 | Define units: ICU, NICU, PICU, isolation, BMT counts | Critical-care brief |
| 2 | Choose layout: open bay / cubicle / single room / hybrid | Layout decision |
| 3 | Size each bed area per spec | Floor area allocation |
| 4 | Plan visibility: nurses' station(s) with sightlines | Station placement |
| 5 | Specify headwall — modular pre-fab | Headwall schedule |
| 6 | HVAC pressure cascade for each unit | HVAC scheme |
| 7 | Isolation and BMT cluster locations | Special-pressure rooms |
| 8 | Family presence — recliner per bed; lounge per unit | Family provision |
| 9 | Multi-faith prayer / counselling | Cultural space |
| 10 | Floor / wall / ceiling finishes specification | Material schedule |
| 11 | Lighting scheme — circadian, dimmable | Lighting schedule |
| 12 | Acuity-adaptable cluster (tertiary) | Future-proofing provision |
References
- ASHRAE (2021) Standard 170-2021: Ventilation of Health Care Facilities. Atlanta: ASHRAE.
- Bartick, M. and Reyes, C. (2012) 'Las dos cosas: an analysis of attitudes of Latina women on non-exclusive breastfeeding', Breastfeeding Medicine, 7(1), pp. 19–24.
- Brown, J., Tomita, R. and Iqbal, M. (2013) 'Designing the ICU of the future', Critical Care Clinics, 29(2), pp. 251–263.
- Davidson, J.E., Aslakson, R.A., Long, A.C., Puntillo, K.A., Kross, E.K., Hart, J., Cox, C.E., et al. (2017) 'Guidelines for family-centered care in the neonatal, pediatric, and adult ICU', Critical Care Medicine, 45(1), pp. 103–128.
- Facility Guidelines Institute (2022) Guidelines for Design and Construction of Hospitals. St. Louis: FGI.
- Gabor, J.Y., Cooper, A.B., Crombach, S.A., Lee, B., Kadikar, N., Bettger, H.E. and Hanly, P.J. (2003) 'Contribution of the intensive care unit environment to sleep disruption in mechanically ventilated patients and healthy subjects', American Journal of Respiratory and Critical Care Medicine, 167(5), pp. 708–715.
- Gulia, A. and Salecha, S. (2019) 'NICU design and developmental care', Indian Journal of Pediatrics, 86(2), pp. 169–174.
- Hamilton, D.K., Orr, R.D. and Raboin, W.E. (2008) 'Organizational transformation: a model for joint optimization of culture change and evidence-based design', HERD, 1(3), pp. 40–60.
- Joseph, A. and Ulrich, R. (2007) Sound Control for Improved Outcomes in Healthcare Settings. Concord: Center for Health Design.
- Kobus, R.L., Skaggs, R.L., Bobrow, M., Thomas, J. and Payette, T.M. (2008) Building Type Basics for Healthcare Facilities. 2nd edn. Hoboken: Wiley.
- Lasky, R.E. and Williams, A.L. (2009) 'Noise and light exposures for extremely low birth weight newborns during their stay in the NICU', Pediatrics, 123(2), pp. 540–546.
- NABH (2020) Standards for Hospitals, 5th Edition. New Delhi: NABH.
- Stiller, A., Sroka, R., Gastmeier, P., Marik, P.E., et al. (2008) 'Single-room contact precautions for the prevention of transmission of multi-resistant organisms', Infection Control and Hospital Epidemiology, 29(5), pp. 408–412.
- Thompson, D.R., Hamilton, D.K., Cadenhead, C.D., Swoboda, S.M., Schwindel, S.M., Anderson, D.C., Schmitz, E.V., et al. (2012) 'Guidelines for intensive care unit design', Critical Care Medicine, 40(5), pp. 1586–1600.
- Ulrich, R.S., Zimring, C., Zhu, X., DuBose, J., Seo, H.B., Choi, Y.S., Quan, X. and Joseph, A. (2008) 'A review of the research literature on evidence-based healthcare design', HERD, 1(3), pp. 61–125.
- White, R.D., Smith, J.A. and Shepley, M.M. (2013) 'Recommended standards for newborn ICU design, 8th edition', Journal of Perinatology, 33, pp. S2–S16.
- Wunsch, H., Gershengorn, H. and Scales, D.C. (2014) 'Economics of ICU organization and management', Critical Care Clinics, 30(4), pp. 703–711.
Author's Note: Critical-care design has matured rapidly over two decades — international tertiary practice has decisively moved toward single-room ICU, single-family-room NICU, and acuity-adaptable patient rooms; Indian practice is in transition, with operational and cost considerations sustaining the open-bay default in most projects. The architect's role is to translate the international evidence into Indian-context decisions — projecting where single-room is justified, where open-bay remains appropriate, and where hybrid configurations make sense. Subsequent guides in this series will go deeper on emergency department design, EBD principles, and HVAC specifics.
Disclaimer: This article is for informational and educational purposes only and does not constitute professional architectural or clinical advice. Critical-care design depends on the specific clinical scope, patient population, regulatory framework, and operational context that must be assessed project-by-project by qualified architects, healthcare planners, and intensivists. Studio Matrx, its authors, and contributors accept no liability for decisions made on the basis of the information in this guide.
Interactive · Critical-care unit configurator
Adult ICU · 12 beds · Cubicle (curtain or glass) · 244 sqm total
Critical-care adults; vent / circulatory support routine.
Layout typology
Beds
Recommended range for Adult ICU: 8-24 beds. Larger units typically split into pods of 8-12.
Bed area
132 sqm
Support area
112 sqm
Total built-up
244 sqm
ACH: 6 (filtered fresh)
Hand-wash: 1 per 4 beds → 3 sinks needed
Isolation: 1 per 8 beds (negative-pressure cube) → 2 isolation cubes
Noise: ≤ 50 dB(A)
Pros · Cubicle (curtain or glass)
- • Better infection control than open bay
- • Some privacy for patients + family
- • Observation preserved with glass
Cons · Cubicle (curtain or glass)
- • Costlier than open bay
- • Curtains carry pathogens — glass preferred
- • Slightly slower team access
NABH preferred
NABH 5th ed. accepts open-bay for secondary care + smaller hospitals; tertiary + private hospitals trending to single-room since the 2020 pandemic.
Areas reference NABH 5th edition + ASHRAE 170-2017 (HC). Local fire-egress and OEM bed-pod dimensions may bump effective area per bed by 10-15%.
Export this guide
Related Guides — Deep-dive reading
Patient Room Typology — Inpatient Room Design Deep-Dive in India
An Architect's Working Reference — Single vs Twin vs Cohort · Same-Handed vs Mirrored · Inboard vs Outboard Bath · Indian Family Attendant Accommodation · Headwall Services · Acuity-Adaptable Rooms · NABH 5th Edition Patient-Centred Design · The Five Decisions That Shape Every Inpatient Floor
Healthcare ArchitectureMaternity & Women's Hospital Design in India
An Architect's Working Reference — LDR/LDRP Models, Obstetric & Neonatal Adjacencies, MTP Act & PC-PNDT Compliance, Postpartum Ward Typology, LaQshya & MusQan Quality Frameworks, State CEA Labour-Room Schedules, and the Women's-Health Service Stack
Healthcare ArchitectureCancer Hospital & Oncology Centre Design in India
An Architect's Working Reference — LINAC Bunkers, Brachytherapy Suites, AERB Type-1 Compliance, Chemotherapy Day-Care, BMT & Isolation, Tumour Board Rooms, Palliative & Hospice Integration, and the Indian Tertiary Cancer Centre Brief
Healthcare ArchitectureRelated Tools — Try Free
Acoustic Privacy (STC) Visualizer
Indian healthcare acoustic visualizer — compare wall assemblies and noise sources, see received SPL after STC attenuation, and check FGI 2018 / IS 1950 / NABH speech-privacy compliance with live dual-canvas waveform.
Acoustic ToolCircadian Light Meter
Patient-centric circadian lighting visualizer for Indian healthcare design — time-of-day × intensity → CCT, melanopic lux (EML / mEDI), melatonin suppression, and an alertness curve. Calibrated against WELL v2 L03 Circadian Lighting Design, CIE S 026:2018, Brainard 2001, and Lucas et al. 2014.
Circadian ToolHealing View Impact Calculator
Evidence-Based Design dashboard quantifying the recovery impact of nature view + daylight factor on analgesic use, length of stay, and HCAHPS patient-experience uplift. Calibrated against Ulrich 1984 (Science), Park & Mattson 2008, and the CHD EBD evidence base.
EBD Calculator